ICD-10-CM Dysphagia (R13):
After Heartburn & Before Flatulence!
By Karen Sheffler, MS, CCC-SLP, BCS-S of SwallowStudy.com
Have you sat through hours of coursework yet for the new ICD-10-CM (Clinical Modification) and ICD-10-PCS (Procedure Coding System)? After 2 1/2 hours of training, I was inspired to investigate further! Do you believe me?
What really happened: I was preparing a blog about all the ways to classify pneumonia, and I thought I would check on how pneumonia was classified in the ICD-9 and ICD-10. I saw how strange the categories of pneumonia were in ICD-10-CM. Then, the hilarious clincher was when I saw that Dysphagia was listed right after Heartburn and before Flatulence and Faecal Incontinence! So, drawing on a little potty-talk mentality, I was inspired!
In this blog I will:
- summarize some of what I learned from my hospital’s training course (Precyse University, 2012),
- uncover how this new thing is NOT so new after-all, and
- explore how ICD-10-CM relates to the Speech-Language Pathologist who works in the field of Dysphagia.
More Codes – More Detail:
Every boo-boo, accident, illness, condition, or disease that a human can get is represented in a code or combination of codes. ICD-9-CM had roughly 13,000 codes, whereas ICD-10-CM has over 73,000 codes. Supposedly, the ICD-10-CM codes are more specific, so that a condition that may have required two codes in ICD-9 now can be reflected in one ICD-10-CM code. There is so much detail in ICD-10 codes that you can tell that it was an initial visit for the person’s injured the left pinky finger, and that the gel-polished fingernail fell off (no, just kidding on the gel polish part!).
A Little History on the ICD-10-CM:
In America, we are gearing up for the big switch to ICD-10! However, this is not even close to being new! Per the World Health Organization’s International Classification of Diseases (ICD) website: https://www.who.int/classifications/icd/en/
“ICD-10 was endorsed by the Forty-third World Health Assembly in May 1990 and came into use in WHO Member States as from 1994. ICD is currently under revision, through an ongoing a revision process, and the release date for ICD-11 is 2018.”
Yes, just as you are training for the ICD-10, what the WHO organization is gearing up for is ICD-11. You can read a report on the external review of the ICD-11 here: https://www.who.int/classifications/icd/externalreview/en/
Why didn’t America adopt the ICD-10 in 1994, like many other WHO nations?
Let’s see, what was America doing in 1994?
Ahh, O.J. Simpson was arrested. Maybe that explains it. Or, the major league baseball strike may have caused severe distress, interfering with our attention to global health matters. People magazine voted President Clinton: “The sexiest man of the year,” after the “sexgate” scandal dating back to his days in Arkansas (yes, before Monica). Did all this cause us to ignore the then-new ICD-10? Unfortunately, we were not paying attention to the 1994 Rwandan genocide either.
Breathe! The ICD-10 is coming to America, finally…
ICD-10 Details for the Therapist:
As therapists, we need to know the diagnosis of our patient before initiating the treatment, ideally with a complete biomedical and pathophysiological set of information. The longer ICD-10-CM codes claim to provide that level of detail in one 7-character code.
In my ongoing quest for more and more clarity in dysphagia, I was excited to see how they coded dysphagia and aspiration pneumonia.
I hope you can feel the excitement to drag yourself through this blog!!
ICD-9-CM Format:
First, let’s recall our codes for Dysphagia in ICD-9-CM. The ICD-9 code used to be all numbers in this 5-digit format:
### . ##
Category . Etiology/Anatomic Site/Manifestation
Remember good old 787.20 for “Dysphagia.Unspecified”? To get more specific with anatomy we used: 787.21 for “Dysphagia.Oral phase,” 787.22 for “Dysphagia.Oropharyngeal phase,” 787.23 for “Dysphagia.Pharyngeal phase,” and so on. We even had 438.82 for “Dysphagia.Cerebrovascular disease.”
So, now with the new ICD-10-CM we will have much more detailed coding for dysphagia, right?
ICD-10-CM code format:
X#X . XXX X
Category with first character always a letter . Etiology/Anatomic site/Severity – Extension
2nd Character is always numeric
Characters 3-7 can be alpha or numeric
Here is an example from my hospital’s training course by Precyse University, 2012:
S06.0X1S
“Concussion with loss of consciousness of 30 minutes or less, Sequela” (not initial visit).
The “X” is a just a placeholder, as the Extension must be the 7th character and gives more info on visit type.
The 10th revision classifies diseases using anatomy. It is called the primary axis (or criterion used to classify a disease). You find the first letter of the 7-digit code by finding what disease category it falls under. For example, a stroke will start with a “G,” as it is in the “Diseases of the Nervous System” category. This can be tricky, though. In the example above, the “S” is in the Injury/poisoning section, rather than in the nervous system. Click Here to browse through the ICD-10-CM codes via the disease systems in the WHO website.
Are you seeing the potential problem for our dysphagia code?
We have been stressing how dysphagia is not a disease in-and-of-itself (See prior blog). It is a symptom of many different diseases, disorders, conditions, injuries, etc. So Dysphagia shows up under a catch-all category called: “Symptoms, Signs and Abnormal Clinical and Laboratory Findings, Not Elsewhere Classified,” and we get the letter R. Click Here to check it out on the WHO website.
Did you find Dysphagia? We are R13. You’ll find it right after Heartburn, and right before Flatulence and Faecal Incontinence! That makes complete sense!
To top it off, this is the only thing it states about Dysphagia:
R13: Dysphagia
Include: Difficulty Swallowing
That is it! Kinda reminds me of when we ask for a reason for doing the Modified Barium SwallowStudy.com on the outpatient coming in, and the doctor’s office tells us only “difficulty swallowing.”
Good thing there are 7 digits total for more detail. We can never just use R13.
New Find: Check out this link to an ASHA Leader article: ICD-10 Implementation: Ready to Code and Bill ICD-10? by Swanson & McCarty. They give examples of R13.10 and R13.19 for the oral phase and the oropharyngeal phase. Yeah!
My advanced search for dysphagia in the ICD-10-CM found the word in 3 more places:
-
“Sideropenic dysphagia” D50.1 (Include: Kelly-Paterson syndrome, Plummer-Vinson syndrome). This extremely rare condition was not familiar to me.
-
Dysphagia is mentioned as an exclusion in the code for “Pain in throat and chest.”
- “Other Somatoform Disorders” F45.8. Somatoform is defined as: Any other disorders of sensation, function and behavior, not due to physical disorders, which are not mediated through the autonomic nervous system, which are limited to specific systems or parts of the body, and which are closely associated in time with stressful events or problems.
ICD-10 lists dysphagia, including “globus hystericus.” under the subheading of Psychogenic dysphagia. You can also find words like Dysphagia functional, Dysphagia hysterical, and Dysphagia nervous in a search. Why are we still using the word “hysterical” in 2015?
Searching through the WHO website makes me feel like our field has a long way to go, but remember, this was made in 1990! 25 years ago!
I also did an advanced search using the word “swallowing,” and here is what came up:
1. “Dentofacial functional abnormalities” K07.5
- Abnormal jaw closure
- Malocclusion due to:
- abnormal swallowing
- mouth breathing
- tongue, lip or finger habits
Exclude: Bruxism (F45.8), Teeth-grinding NOS (F45.8)
2. There are codes when things are swallowed that should not be swallowed:
- Corrosion of other and unspecified internal organs.
- Assault by corrosive substance.
- Corrosion of other parts of alimentary tract.
- Foreign body entering into or through eye or natural orifice.
- Accidental poisoning by and exposure to other and unspecified chemicals and noxious substances.
Here is another useful code!
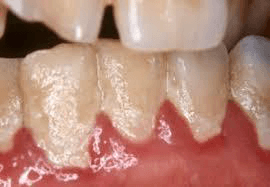
There is a code for the crud that builds up on the teeth of our patients who do not get oral care in institutions. K03.6 – my new favorite code! This stands for “Deposits (accretions) on teeth,” which includes dental calculus and staining of teeth. Accretions is an older term for accumulation of foreign material on teeth, but now called deposits (per www.medical-dictionary.thefreedictionary.com).
The list under this category goes into gory detail about the color of the staining. Is it orange, black, from tobacco, from a betel nut, or Materia alba? My new favorite word! See, this search was worth it!
Materia Alba: white cheeselike accumulation of food debris, microorganisms, desquamated epithelial cells, and blood cells deposited around the teeth at the gumline (per www.medical-dictionary.thefreedictionary.com).
How about aspiration pneumonia?
A search for aspiration pneumonia revealed inadequate and confusing terminology in the J69 codes. The “J” is under “Diseases of the Respiratory System.” (Note that Neonatal aspiration syndromes (P24.-) are under the letter “P” for “Certain Conditions Originating in Perinatal Period.”)
Scan through Diseases of the Respiratory System to find the heading: “Lung diseases due to external agents.” Then you can find J69 subsection, which is “Pneumonitis due to solids and liquids.” Fortunately, it does indicate that you can add a “external cause code” (Chapter XX), which may help to clarify the code. I hope.
On the WHO website, here is how the section breaks down word-for-word:
“Pneumonitis due to solids and liquids:
J69.0 Pneumonitis due to food and vomit
Aspiration pneumonia (due to):
- Not otherwise specified (NOS)
- food (regurgitated)
- gastric secretions
- milk
- vomit
Exclude: Mendelson syndrome (J95.4)
J69.1 Pneumonitis due to oils and essences
Lipid pneumonia
J69.8 Pneumonitis due to other solids and liquids
Pneumonitis due to aspiration of blood”
That brings up a few questions:
- Why are we mixing up pneumonitis and pneumonia?
- Why does J69.0 say pneumonitis in the heading, but aspiration pneumonia under the heading?
- Why is the term “aspiration pneumonia” only found in one code, which actually incorrectly labels it as a pneumonitis?
- Why does the J69.0 heading say “food,” but the bullet point specifies that the food must be regurgitated and then aspirated?
- Why is there a bullet for “milk,” but no bullet point under “aspiration pneumonia” for other liquids?
- Why does the J69.8 heading say “other solids and liquids,” but then specifies only the aspiration of blood?
So, while dysphagia and pneumonia research use helpful terms like Dysphagia-Related Aspiration Pneumonia and HealthCare-Associated Pneumonia, our new ICD-10-CM codes will reflect strange-arbitrary categorizations.
I think I should stop now!
I hope this trip through ICD-10-CM was as enlightening and as frustratingly funny for you as it was for me. Remember, laughter is the best medicine! Maybe we should set our sights on ICD-11!
What does this all mean for me as a therapist?
Fortunately there are medical coders and ICD-10 specialists out there to help, but it is the therapists’ job to document well and select the most accurate diagnosis code under which to treat.
- When billing therapy services, the diagnosis needs to be specified.
- Always use the most specific code available.
- Code selection needs to be based on objective evidence that most accurately and completely describes the patient’s condition(s).
- All conditions that coexist at the time of your therapy encounter, which directly affect your therapy, should be documented and coded. In other words, if you are treating two or more conditions, then include the codes to reflect those conditions/diseases. But watch out, what used to be two codes in ICD-9-CM may now have one more specific code in ICD-10-CM.
- Document, document, document! Documentation needs to reflect the diagnoses you are treating. Combination codes may also be a diagnosis with it’s associated complication or manifestation, but your paperwork needs to reflect that level of detail. Think like ICD-10-CM with a focus on: anatomy, etiology/causes, site of the condition, and severity.

The better your documentation is, the more accurate and specific the medical coders can be. The more specific you are, the more likely your evaluations/treatments will be covered.
Your thorough documentation will also be crucial when medical coders build the inpatient 7-digit procedural codes of ICD-10-PCS (Procedure Coding System, which replaces ICD-9-CM Volume 3). This is a brand new coding system to reflect every procedure that is performed on inpatients! Don’t worry, I won’t go into the ICD-10-PCS detail, yet…
Hope others will share ICD-10 stories! Do it now, before ICD-11!
If you still want more, please click here for the ASHA store for many ICD-10 products.