
Thank you for your interest in:
Oral Care & Aspiration Pneumonia Prevention
Here you will find links to my four-part blog series on
Oral Hygiene and Aspiration Pneumonia Prevention and More!
by Karen Sheffler, MS, CCC-SLP, BCS-S of SwallowStudy.com
I have shared Part I below.
Top SwallowStudy.com Links in Oral Care / Oral Hygiene:
- Click on these links to see Part II, Part III, and Part IV.
- See also my 5th blog on the topic: “It’s Alive! Oral Microbiome.”
- Check out my guest bloggers: Joanne Yee, MS, CF-SLP & Dr Nicole Rogus-Pulia, PhD, CCC-SLP, who wrote “The Saliva Puzzle: Saliva Production & Swallowing.”
- Open this pdf to share oral care procedures with staff: Oral Care Procedures for Aspiration Pneumonia Prevention
- The Oral Health Assessment Tool (OHAT) allows healthcare providers to screen for the need for a dental examination. (Chalmers, et al., 2005).
Updates: We need to start thinking more seriously about oral care, as it is actually part of a person’s infection control program. Calling it “oral care” may have lead to this crucial prevention strategy to be overlooked or forgotten in busy hospital and facility routines. Oral infection control and oral decontamination are crucial aspects of preventing hospital acquired infections (HAI), such as aspiration pneumonia. Please see my March 25, 2021 webinar hosted by the National Foundation of Swallowing Disorders (NFOSD) titled: More Than Oral Care – Let’s Talk Oral Infection Control (register now or see the recording after the webinar).
Part 1
Oral Hygiene and Aspiration Pneumonia Prevention:
10 trillion microorganisms versus your toothbrush!
by Karen Sheffler, MS, CCC-SLP, BCS-S of SwallowStudy.com
Inspired by the presentation: “Dental Perspectives on Aspiration Pneumonia Causes and Management” by Kennneth Shay, DDS, MS, Dentist and Gerontologist Department of Veterans Affairs: Office of Geriatrics and Extended Care. Presented at the ASHA Healthcare & Business Institute, April 12, 2014, Las Vegas, NV

The biggest hole in the body can harbor many bacteria.
“The mouth is dirty,” Dr Kenneth Shay stated frankly – and – it is “the biggest hole in your body!”
I hope I don’t gross you out! So finish eating, go brush your teeth, floss, use mouthwash, and then come back…
OR
If it is early morning and you haven’t brushed your teeth yet, then scrape the gunk off your teeth with your fingernail. You may have found 10 billion microorganisms in that cubic millimeter.
There are 1 trillion to 10 trillion microorganisms in your mouth.
Dr. Shay recommended the simple tool of a toothbrush for oral infection control in healthcare. Simply brushing your teeth can get rid of that nasty bacteria film in your mouth. It can also prevent “some of that schmutz” from getting into your lungs. If you are having trace aspiration (saliva, food, and/or liquids getting into your lungs), try to make what gets into your lungs less nasty. You can prevent pneumonia with proper oral care.
Pneumonia due to poor oral care is a major avoidable infection, per Shay.
Ross & Crumpler (2006) noted that despite strong evidence in the literature on the role of brushing the teeth in preventing aspiration pneumonia, medical staff continue to view oral care as a comfort measure and only use foam swabs.
“Toothette sponges are wimpy,” stressed Shay. They don’t get the gunk (plaque) off the teeth. Plaque is sticky. If not removed, it hardens into tarter (also known as calculus). Then a visit to the dentist is needed to scrape it off (called debridement). And, do we even dare to ask for people to receive flossing!?
Why is the mouth forgotten in healthcare?
We wash our hands and wear gloves before serving food to prevent spreading harmful bacterial infections. As of 2020, frequent hand washing has become even more routine in our new-normal-pandemic days. So, why not frequently brush the teeth of a dependent elder in order to prevent a bacterial pneumonia?

We help dependent elders with many activities of daily living. Brushing the teeth is just as important as toileting.
We help him go to the bathroom many times a day. So why don’t we help brush his teeth?
I’ve heard some nurses say they are squeamish about the mouth! It makes them gag! Well, we should be gagging over the health and financial costs of neglecting the mouth.
This simple prevention technique of brushing costs pennies a day against the cost of a pneumonia. Based on CDC numbers from 2011, there were 157,500 Hospital Acquired Aspiration Pneumonia infections that year. CDC states the average added cost of ONE hospital acquired pneumonia is $22,875. This equals over 3 billion dollars! See: https://www.cdc.gov/hai/surveillance/ That cost is certainly a low number, and it likely represents just the pneumonia itself. What about the Medicare penalties for causing harm to the individual with a hospital acquired infection (HAI)? What about the increased length of stay in the ICU and hospital, potential prolonged duration of intubation, IV antibiotics, and the need for post-acute care in a skilled nursing facility/rehabilitation center rather than being discharged home?
Shay also speculated that one reason why the mouth is the forgotten part of medicine is that the medical profession began to ignore it about 150 years ago. This was when the dental profession split from the medical profession. Then to make matters worse, in 1965, dentistry said “no thank you” to Medicare. Read more of this history here:
Why are we not protecting this wide open gateway to the body?
Imagine your gingival space between the tooth and gum as a huge parking lot. Germs love these 1-3 millimeter deep parking spaces. If germs park in the gingival space for more than 24 hours, they become calcified into plaques. Bacterial loves to stick to it. Brushing removes plaque. No brushing leads to a build-up of plaque in the gingival space and inflammation (gingivitis).

Gingivitis
It only takes 48 hours of hospitalization in a critically ill patient to change the bacteria from the usual gram-positive streptococci to gram-negative microorganisms (nasty pathogenic bacteria that cause pneumonia).
Maybe we don’t brush our patients teeth because the gums bleed? Blood is okay, per Shay, even if you are on a blood thinner. Shay stated that bleeding is a sign that you need to brush more. It is due to the inflammation, and regular brushing will prevent bleeding. Shay warned that bleeding is only risky if the patient has a blood disorder or disease that causes excessive bleeding.
Most cases of gingivitis do not progress to the more serious periodontitis or to aspiration pneumonia.
Immune-compromising events can cause an autoimmune response that can lead to periodontitis, per Shay. Examples of immunocompromising events are not only critical illness; they could be the following:
- life stressors,
- flu,
- depression, and
- pregnancy.
Periodontitis is inflammation caused by bacteria that affect the attachment between the tooth and the bone. It is an irreversible destruction of the supporting tissues (periodontal ligament to alveolar bone).
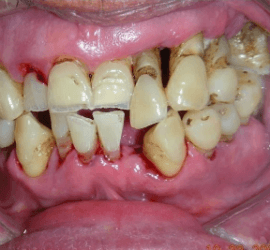
Periodontitis with gums receded and more space for the gram-negative bacteria to colonize surfaces
Then bone-absorbing cells eat away at the bone. The bone will not be regenerated. The periodontal pocket that is formed creates a larger “parking garage” of 6-8 millimeters deep.
Additionally, “there is more surface area to collect gunk,” said Shay.
As the gums recede and the bone wears away, the cementum is exposed. Cementum is not hard and smooth like enamel. It is rough, and bacteria can stick to it easier than enamel. Cementum has a higher organic content, and is more susceptible to decay when there are changes in salivary pH. Here is the pH scale, with healthy saliva at a 6.
Lots of gram-negative anaerobic bacteria can park there! Pathogenic microorganisms. “These are the same things that cause aspiration pneumonia,” stated Shay.
Bottom Line = Brush!
But what if I can’t use a toothbrush on my patient?
First, I would ask, Why? Why do you think you cannot use a toothbrush? Is it soft? Does it have a suction attached? If the reason is mucositis and oral pain, then make sure to refer to treat these right away. Some bleeding is okay, as it shows that the mouth really needs to be brushed more often. Some people with Dementia and cognitive challenges may be resistant, so try to do hand-over-hand holding of the toothbrush with them to bring back the automaticity of the task.
Ransier, A., Epstein, J.B. Lunn, R., & Spinelli, J. (Cancer Nursing, 1995) found that a chlorhexidine-soaked foam brush could reduce plaque and gingivitis as effectively as a toothbrush. They speculated that this may be helpful when a patient has mucositis and mouth pain. However, the study was done on healthy individuals in a 2-week trial only.
Research on Chlorhexidine-Gluconate (CHG) has been only “so-so” in decreasing aspiration pneumonia risk, per Shay.
The positives on Chlorhexidine are:
- broad-spectrum antibacterial
- continues it’s action in the mouth for 12 hours (substantivity)
Even in patients with NO teeth, we need to debride the mouth. Pathogens can still colonize the oral mucosa. Wipe the inside of the mouth, and scrub the tongue as a means of oral care and prevention. Hydrogen peroxide on the foam swabs does not have a detergent-action and deriding action like toothpaste on a toothbrush.
Thank you for reading Part I of Oral Hygiene and Aspiration Pneumonia Prevention.
*******
Here are some of those links again:
1. How to screen the mouth for the need for a dental consult: The Oral Health Assessment Tool (OHAT) from Chalmers, et al., 2005.
2. Read more on Chlorhexidine, Hydrogen Peroxide and how to provide oral care:
Part IV (How to Perform Effective Oral Care)
Oral Care Procedures for Aspiration Pneumonia Prevention (pdf)
3. Part II (Where I discuss the saliva and salivary pH by comparing the mouth of a critically ill person to the disturbance of the ecosystem after Mount Saint Helen’s volcano.)
4. Part III (Where I discuss the many pathogens that may colonize the mouth and take a trip it into the lungs. Ready to travel, anyone?)
5. “It’s Alive! Oral Microbiome.” (Where I compare the delicate microbiome of the mouth to that of a dessert!)
Yes, I have loved to travel, and I hope you will feel like you are traveling while reading these blogs. Hopefully we will safely travel again soon!
6. Please see my March 25, 2021 webinar hosted by the National Foundation of Swallowing Disorders (NFOSD) titled: More Than Oral Care – Let’s Talk Oral Infection Control (register now or see the recording after the webinar).
(Last update: March 2021)


