Wallenberg Syndrome
Also known as Lateral Medullary Syndrome or Lateral Medullary Infarct
by Karen Sheffler, MS, CCC-SLP, BCS-S of SwallowStudy.com
I want to share my literature review I did when my son had just started at preschool, and I had a little more time on my hands! The inspiration was not only from my patients with Wallenberg Syndrome, but also from hearing James Coyle, PhD, CCC-SLP, BCS-S speak at an ASHA convention. He was advocating for clinicians/dysphagia practitioners to do research. This inspired me to perform an extensive literature review and present the information in a 2-hour lecture at the ASHA convention in San Diego in 2011.
The literature review (LMS – Wallenberg Syndrome Literature Review and Case Studies) is extensive, at over 60 pages double spaced! I’m sure there have been recent publications since I completed the writing several years ago. I look forward to comments from readers. Please let me know if you have seen publications on this topic that are not in my reference list below. I welcome all feedback and discussion.
Wallenberg Syndrome Literature Review Abstract:
A lateral medullary infarction (LMI) or stroke typically creates a cluster of symptoms also known as lateral medullary syndrome (LMS) or Wallenberg syndrome. It is the most common type of a brainstem stroke, and it presents completely differently than a cortical stroke (aka, a cerebral vascular accident [CVA] that occurs higher up in the person’s cortex). There is a need to increase public awareness in this type of stroke, as the cluster of symptoms include nausea and vomiting, which may be mistaken for a gastrointestinal infection or flu. The effects of this infarction need not be devastating. With early identification and treatment, including early swallowing evaluations, the medical team can prevent aspiration pneumonia, intubation, and death from pneumonia.
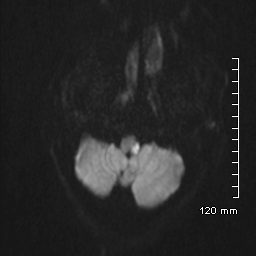
MRI: Diffusion Weighted Image (DWI). This shows the restricted diffusion in the left lateral medulla as a bright white signal.
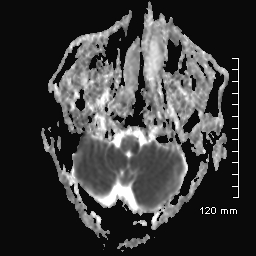
MRI: Apparent Diffusion Coefficient (ADC map or sequence), showing a dark-low signal. The bright signal above plus this low signal = restricted diffusion, which = acute stroke.
The goals of the paper:
(a) Provide a review of the literature of LMS,
(b) Discuss the symptoms and challenges of differential diagnosis,
(c) Analyze the dysphagia research in LMS, especially how it relates to the central pattern generators (CPG) for swallowing,
(d) Discuss the pharyngeal, laryngeal, and esophageal aspects of the dysphagia in LMS; and to
(e) Review recovery, prognosis, and treatment options.
Finally, two cases are presented that illustrate points such as:
- the younger age of onset of LMS in comparison with most stroke populations,
- symptomatology,
- the need for early identification,
- the need for instrumental evaluations of swallowing,
- therapy techniques and expected outcomes.
LMS patients tend to show rapid and steady recovery of their swallowing function within days to months. The subjects of the two case studies at the end of this paper made significant progress in swallowing based on a comparison between the evaluations at two days after the stroke and at just six days later.
The important message is that with any suspected brainstem infarction, the patient should remain NPO until the swallowing is fully evaluated. In the second case presented at the end of the article, early identification of the infarction by the team prevented major aspiration and intubation (which had occurred with the first case).
Click below for the free pdf downloads of the full text and references:
LMS – Wallenberg Syndrome Literature Review and Case Studies
LMS-Wallenberg Syndrome Reference List
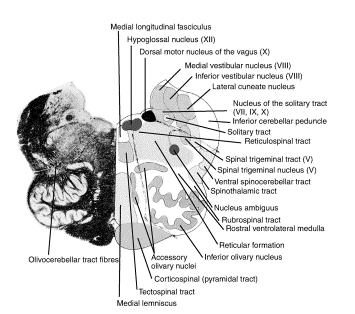
Cross section of the medulla. When the Lateral Medullary Infarct is in the dorsal-rostral aspect of the medulla, it can really affect voice and swallowing.
Historical Perspective on Wallenberg Syndrome:
Click on this link below if you would like to read a fascinating paper written in 1811 describing a patient with Wallenberg Syndrome:


I am in fact grateful to the owner of this website who has shared
this great piece of writing at here.
I would love to see any additional research on Wallenberg Syndrome, as I have this and it is difficult to find any information on research and potential reversal or cure.