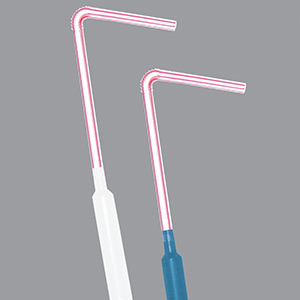
SafeStraw by Bionix
SafeStraw: A Volume Limiting Drinking Aid
by Bionix Medical Technologies
These straws deliver only 6.2ml when the patient sucks on the straw. A smaller sip volume may be safer and prevent aspiration in people with dysphagia.
Great when a patient has difficulty remembering to take a small sip.
Need to have enough strength to sip from straw. Not for everyone. Ask your Speech-Language Pathologist. Individuals can purchase these from Bionix Health At Home.
Note: I do NOT receive any commission from a click or a purchase. I have received NO financial compensation for writing this product review.

TAKE A SMALL SIP!
Product Review: SafeStraw by Bionix
by Karen Sheffler, MS, CCC-SLP, BCS-S of www.SwallowStudy.com
Straw Drinking & Dysphagia: A Background
Do you find yourself choking when you are chugging your drinks?
Does fast drinking from a cup or straw make you cough, like liquid is going down the wrong pipe?
Maybe it is. Maybe a Speech-language Pathologist (SLP) needs to evaluate your swallowing function. See post on “How do I know I need a swallow study?”
Speech-Language Pathologists (SLPs) specializing in difficulty swallowing (dysphagia) have lots of tricks to make it easier to swallow. Frequently, SLPs recommend the strategy of taking small sips, based on the person’s swallow study.
However, is that realistic?
Lawless, et al., (2003) noted that average cup sips are 25ml or 20ml for healthy men and healthy women, respectively. Recently, Steele, et al., (2015) found that when given a full cup of water, people tend to take sip sizes of 16ml, on average.
We may note on a person’s swallow study, that a teaspoon-size sip (5ml) of a thin liquid is safe, but who drinks out of a spoon? How would that affect the person’s hydration and quality of life?
We also may report on a swallow study that a small sip by cup prevented liquids from going down the wrong way, but who will sit next to that person all day and everyday to remind him to take small sips? If a 25ml size sip is his automatic-natural way of drinking, then a 5ml sip is a big change.
Furthermore, the swallow study may show that liquids go down the wrong way when taken rapidly by a straw (sequential drinking). However, it tends to be challenging to get staff and family to remember to avoid straws.
What if the person prefers to drink out of a straws? What if the dependent patient in the hospital is easier to feed when using a straw?
A straw may make it easier to get the liquid in the mouth. Veiga et al., (2014) found that it was easier for healthy elderly adults to take sequential sips via a straw from an oral point of view. The liquid did not spill out of the mouth as much as with sequential cup drinking. This study was done with healthy elderly with a mean age of 72.8 years. None of the healthy elderly had airway compromise, meaning no liquid got into the top of the airway/laryngeal vestibule (penetration) or below the level of the vocal cords (aspiration), but only 100ml was taken.
Do people aspirate more via straw than cup? Daniels, et al., (2004) studied healthy young and elderly individuals. They found inherent problems with sequential straw drinking that increase risks. Sequential straw drinking, no matter young or older, tends to allow the volume of liquid to drop too low in the throat before the swallow (i.e., bolus head was inferior to the valleculae in the hypopharynx before the onset of the swallow in 66% of adults). Additionally, older adults (ranging in age from 60-83 years old) had more airway compromise (penetration and aspiration) during sequential drinking of 300ml.
These studies were on healthy elderly. What if the elderly person is weak, lethargic, confused and sick? Is straw drinking safe and possible? This is why a formal swallowing evaluation may be needed by an SLP to rule-out aspiration and dysphagia, and to determine the best safe-swallow strategies.
The amount of risk could be significantly higher in people with dysphagia (difficulty swallowing). Your Speech-Language Pathologist (SLP) can fully evaluate your swallowing function with a Modified Barium SwallowStudy.com (aka, MBSS or Videofluoroscopic SwallowStudy.com – VFSS) or a Flexible/Fiberoptic Endoscopic Evaluation of Swallowing (FEES). Depending on your specific structural and physiological swallowing difficulties, the SLP may recommend small sips to prevent penetration and aspiration of liquids into your airway. See post on “How is my swallow evaluated.”
Sometimes thickened liquids are recommended, especially if a person cannot modify his/her sip size and follow safe-swallow strategies. However, thickened liquids may effect the person’s intake and quality of life.
Potentially, a device that modifies the sip size for the patient could keep the patient off thickened liquids and enjoying any regular thin liquid beverage safely (per testing by an SLP and your medical team’s advice). See *Key Points section below.
SafeStraw Product Review for People with Dysphagia to Liquids:
The specific device I tested was the SafeStraw: A Volume Limiting Drinking Aid, by Bionix. For individual purchases of the straws, go to: Bionix Health At Home website and check out the Product Directory. Again, I receive no financial compensation for this recommendation.
I particularly like the White / SafeStraw Drinking Aid for Thin Liquid. I found the sip size was consistent when drinking water via the SafeStraw. The sip volume was equal to a full plastic teaspoon (roughly 5ml in a medicine cup). When SLPs test swallowing with X-ray or endoscopy, one of the methods to test liquids is via a plastic teaspoon, but some spoons are bigger than others.The testing per the company is obviously more accurate, and they report consistent 6.2 ml size sips. The company describes how it works as follows:
SafeStraw Pluses:
- Lightweight: put it in your pocket when you go out to eat.
- Thin: drop it into any water/juice bottle with a narrow top.
- Short: no one will see it. It just looks like part of a normal straw, especially the White/SafeStraw Drinking Aid for Thin liquid. (Whereas, the Blue/SafeStraw Drinking Aide for Thick Liquid is bright blue and more visible. However, the color coding is needed as the floats are different materials.)
- Versatile: you can attach a normal plastic drinking straw to the top of it.
- Adaptable: Cut any straw to attach a smaller straw to the top of the device. A shorter straw may make it easier to drink: reducing the amount of pressure you need to build up in your mouth and reducing the amount of time you need to be sucking. (Cichero & Murdoch 2006; Groher & Crary, 2010)
- Less waste: The device is NOT a one-time use; therefore, it is more affordable and less waste than some adaptive straws on the market.
- Easy to take apart and clean: It comes assembled, but there is an assembly diagram in the package. Don’t loose the float piece when you take it apart. You can soak all parts it in hot soapy water. I would imaging you could run rubbing alcohol through it to disinfect, and then thoroughly rinse.
What do you need to know about SafeStraw?
- You cannot take sequential sips from this device. It prevents rapid chugging to hopefully improve your swallowing safety. It is like a little helpful reminder! However, if the person gets easily agitated, this may increase frustration.
- Wait time between sips: Unfortunately, you cannot take another full sip until the float falls back to the bottom of the cylinder. This takes 3 seconds for the White/SafeStraw Drinking Aid for Thin Liquid.
- Your first sip when you first start your drink is a priming sip, and you may not get any liquid at all. Once it is primed (i.e., liquid in the chamber/cylinder), the rest of the sips will be consistent for the white SafeStraw for thin liquids.
- I found the Blue / SafeStraw Drinking Aid for Thick Liquid to be a bit challenging and too variable. I tried it on a “nectar thick” milkshake. The metal float did not consistently drop back down. A shorter straw did not help. I discussed this with a representative from Bionix, and he noted that the Blue SafeStraw is made with a food-grade-rust-proof stainless steel float. It is supposed to be heavier than typical nectar thick liquids. However, there may be too much variability in the true viscosity or thickness of nectar thick liquids, as well as solid particle/fat content. For example, my smoothie made with yogurt, and almond milk, as well as my vegetable and juice smoothie, really made the float get stuck. Whereas, my pudding and milk smoothie may have been thinner and the float fell to the bottom of the cylinder easily.
Note: SafeStraw instructions indicate that it takes 6-9 seconds for the float to sink to the bottom with the Blue / SafeStraw Drinking Aide for Thick Liquid.
SafeStraws are good for thin liquids, except carbonated liquids (use the white one – SafeStraw Drinking Aide for Thin Liquid).
The Blue SafeStraw Drinking Aid for Thick Liquid is made for a mildly-thick or nectar thick liquid, but not for thicker liquids (i.e., NOT for moderately to extremely thick liquids, like “honey” thick or “pudding” thick liquids).
* Key Point *
Not every patient with dysphagia will be able to use this device, as some people may have weaknesses or cognitive deficits that prevent them from being able to use a straw at all. The company notes that the SafeStraw is for “deficient oropharyngeal or oral motor skills;” however, some types of oral-motor weakness and oropharyngeal dysfunction will make it hard to use this straw device.
What is required for straw drinking?
- First of all, the patient has to recognize what to do with a straw. (Unfortunately, in very advanced Dementia, people loose the ability to recognize what to do with common utensils like straws.)
- Adequate lip strength to seal around the straw.
- Ability to build up intraoral pressure, which requires:
- Good soft-palate closure (aka, velopharyngeal closure) to block off the nasal cavity.
- Good swallowing-breathing coordination.
Summary:
Ultimately, it is your medical team and your Speech-Language Pathologist who will help you determine if you are a good candidate for SafeStraw. Why not bring the SafeStraw devices with you to your instrumental evaluation and drink thin and thick barium contrast through it? Just perform many trials with the SafeStraw to make sure it is safe and consistent (i.e., 6 trials with a thin liquid). It will be easy to rinse the barium out when you are done!
I am glad to test a device that can really have an impact on a patient’s safe hydration, quality of life, aspiration prevention, and potentially aspiration pneumonia prevention, especially if it can help the patient avoid thickened liquids and drink regular liquids. We always want to see our patients on the “least restrictive fluid” (i.e., thinnest liquid) possible. This device could be a big help!
If you need thickened liquids, I can recommend this company to make your purchase: